Q6. Blount’s disease is present as
1. Genu recurvatum
2. Genu varum
3. Genu Valgum
4.
Answer - 2. Genu Varum
Refrence - Turek's Ortho
TIBIA VARA (BLOUNT'S DISEASE)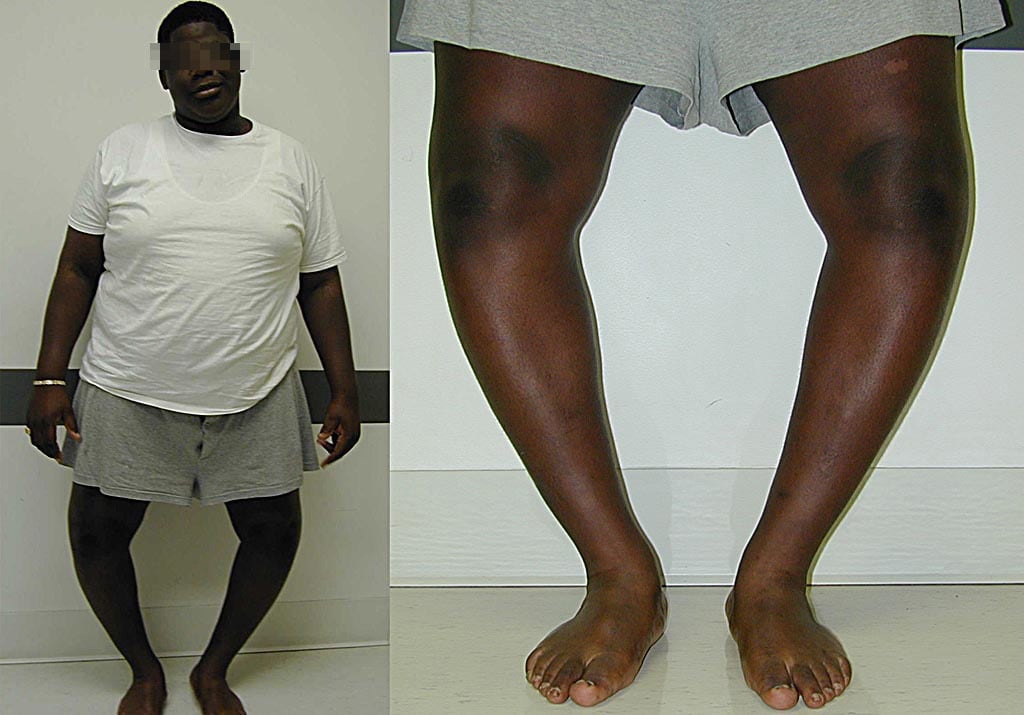
 Tibia vara is the most frequent nonphysiologic cause of genu varum in children and adolescents
Tibia vara is the most frequent nonphysiologic cause of genu varum in children and adolescents. It is considered to be a developmental condition, which affects posteromedial aspect of the proximal medial tibial physis, resulting in a progressive varus deformity. Biopsy of the lesions reveals disorganized physeal cartilage with abnormally large groups of capillaries, densely packed hypertrophic chondrocytes, and islands of almost acellular fibrous tissue. Both fibrovascular and cartilaginous reparative tissue can be found at the physeal-metaphyseal junction. Infants affected by this condition are usually of black or Mediterranean origin, often have a history of early walking, and are in the upper percentile of weight for height. Examination of the child with tibia vara reveals an angular deformity discernable just below the knee. In contrast, young child with physiologic genu varum will have a more gentle curvature of the entire extremity. A lateral thrust, indicating laxity of the lateral ligamentous complex, may be seen in children over the age of 3 with tibia vara.
It is generally subdivided into infantile and late onset forms. Infantile Blount's disease may be difficult to diagnose in its early form until 2 years of age, when the radiographic changes suggestive of infantile tibia vara are more evident (Figure 18-5). The Langenskiöld radiographic staging classification reflects the progression of tibia vara in untreated cases. The natural history of untreated cases is to progress to complete medial physeal arrest, which can occur by the age of 6 (Figure 18-6). In such an event, subsequent treatment is difficult, because both angular deformity and tibial shortening must be addressed. Other radiographic criteria have been developed, such as the metaphyseal-diaphyseal angle for the early diagnosis of Blount's disease. Some children with metaphyseal-diaphyseal angles described as compatible with infantile tibia vara (an angle of 16° is currently accepted) spontaneously improve without treatment; at the present, this differentiation continues to be very difficult in the early Langenskiöld stages.
FIGURE 18-5. Anteroposterior radiograph of a 3-year-old boy with infantile tibia vara. Prominent beaking of the medial metaphysis and varus angulation at the epiphyseal-metaphyseal junction are evident.
The role of bracing remains unclear; however, brace management in patients younger than 3 years old may be successful in correcting the mild deformity. Obesity, instability, and delayed bracing are considered as risk factors for failure. Early valgus osteotomy before 4 years of age is strongly recommended to minimize deformity of the proximal medial physis. With this in mind, overcorrection into 5 to 10° valgus angulation beyond normal should be the goal. The pathology of late onset tibia vara between the ages of 6 and 13 is similar to that of
P.579
infantile tibial vara; however, because growth at the tibia is closer to maturity in the adolescent, bracing is not effective. Various techniques, including plate, monolateral, or circular external fixation, have been described to maintain position after osteotomy. Use of rigid external fixation with acute or gradual correction allows accurate alignment of the lower extremity and prevents complications such as nerve palsy, compartment syndrome, overcorrection, or undercorrection. For those adolescent patients with significant growth remaining, consider selective lateral epiphysiodesis. The rate of correction following this procedure has been reported to be 4° per year.

 Home
Home








